My Inspiration for Better Healthcare
Quite often we start showing interest in something, when that something affects us personally.
For me, it was my mom’s stroke, that happened in 2009, that made me painfully aware of just how fragmented our current healthcare system is and that patients with chronic conditions can easily get lost in it.
I can still remember that moment when I learned about my mom’s stroke.
I was at work. Busy day. I was in meetings most of the day, so I didn’t check my phone at all. When I finally checked it – I had millions of missed calls and voicemail messages from my family members. I quickly checked the last message and learned the news.
I remember feeling confused, helpless and physically sick all at the same time.
I didn’t know much about stroke, so I had no idea what to expect.
The first image – my mom’s face looks almost unrecognizable, because of her crooked mouth.
I arrived at the time when her doctor was doing an examination and she was trying to reach her nose with her finger, but couldn’t. My brother, seeing my reaction, pulled me to the side saying that this is much better than before – she couldn’t even lift her left arm when he arrived. I felt like I needed to sit down.
You might think that this was the beginning of our long journey into healthcare. It wasn’t!
For 2 years prior to my mom’s stroke, we’d been to a number of hospitals and specialists with a variety of symptoms that were changing over time, yet nobody could give us a proper diagnoses. In those 2 years, I didn’t hear a word “Stroke” even once.
You might think that the news of my mom having a stroke was the worst thing I’ve learned that year. It wasn’t! The worst thing for me was learning that her stroke was totally preventable!
It took doctors 2 years and a stoke to finally give my mom a diagnoses – Atrial Fibrillation.
What is Atrial Fibrillation?
 Here is what you can learn about AFib on stroke.org.
Here is what you can learn about AFib on stroke.org.
“Atrial Fibrillation (AFib or AF) is an irregular or “racing” heartbeat that can cause blood to collect in the heart and form a clot, which can then travel to the brain and cause a stroke.”
AFib-Stroke Connection is well known.
“AFib raises a person’s risk for stroke by 500%, and most AFib-related strokes (75%) can be prevented.”
A 2013 study published in Circulation revealed that 33.5 million people around the world have AFib. That’s about 0.5% of the world’s population.
AFib is an expensive condition.
According to the American Heart Association, treatment for AFib costs about $26 billion dollars a year in the United States alone. When compared to other patients, people with AFib are admitted to the hospital at double the rate.
Treatments for AFib
“Most AFib-related strokes can be prevented with anti-coagulation treatments, yet up to two-thirds of AFib patients who had strokes were not prescribed anti-coagulants or blood thinners. Anti-coagulation can reduce the risk of a first stroke by 60 to 80%.” (stroke.org)
My mom was one of those two-thirds of AFib patients that wasn’t prescribed anti-coagulants in time. Something as simple, as aspirin, would’ve significantly reduced her risk of stroke.
So what happened?
I asked myself this question many times since.
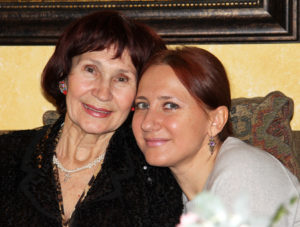 Why, in 2 years time, did no one notice something and give my mom a proper diagnoses? Why, with so many symptoms and doctor visits, was she not taken seriously? (One doctor told my mom to relax – go home and drink some tea; another one suggested we check her head, thinking she is imagining her symptoms.) Where is Dr. House when you need him?
Why, in 2 years time, did no one notice something and give my mom a proper diagnoses? Why, with so many symptoms and doctor visits, was she not taken seriously? (One doctor told my mom to relax – go home and drink some tea; another one suggested we check her head, thinking she is imagining her symptoms.) Where is Dr. House when you need him?
Here is what I think is the reason why my mom’s AFib was missed by so many doctors.
Many chronic conditions and diseases (incl. AFib), take decades to develop, and are entangled with hundreds of dietary, lifestyle, genetic & environmental factors. Their detection requires continuous monitoring of multiple data points over a long period of time. It also requires information sharing among all healthcare providers.
None of this was happening in our case.
My mom would go to one doctor with one symptom, like a burning sensation in her chest, and then a few days later she’d go to another doctor with another symptom – extreme fatigue. Both doctors would order similar (or exactly the same) tests and none of the info would be shared between them. Then my mom would go to an ER with severe chest pain. The ER doctor also doesn’t have access to her previous doctors’ notes or their test results, so he’d order more tests.
Basically, nobody had a complete picture of my mom’s changing health situation, even my mom. She didn’t have a copy of her health records either, which would be extremely valuable in emergency situations.
Plus, nobody was actively monitoring her symptoms over time to notice how her condition and her quality of life slowly deteriorated.
Our current healthcare system is simply not setup for this kind of monitoring and information sharing, making early detection of chronic disease virtually impossible. That’s why people learn that they have cancer at stage 4 or they have AFib after after they have a stroke.
The whole thing to me looked like a giant puzzle, where each person was looking at one piece of a puzzle at a time, never seeing the rest.
Working in IT and the banking industry for many years, I knew how technology was transforming other industries, and that we have all the technology we need to do a much better job in healthcare when it comes to detection of chronic conditions.
– We have fast computers that can handle “Big Data”
– Wearables can now monitor anything from sleep to heart rate in real-time
– Machine Learning allows us to reveal insights from large amounts of unstructured data
If we can access our consolidated banking information on the go, we should be able to do the same with our health records. And if we can predict perfect sunsets, we should be able to predict (and prevent) strokes.
Those are just some of the changes that I want to see in the Healthcare. And I want to see them in my mom’s life-time.
That’s my inspiration behind Dateva.





Pingback: kamagra za nižší cenu
Pingback: discount rifaximin cheap sale
Pingback: how to order xifaxan cheap in canada
Pingback: buying staxyn purchase from uk
Pingback: online order avodart purchase from uk
Pingback: discount itraconazole
Pingback: ordering fildena cheap from india
Pingback: get gabapentin purchase australia
Pingback: price of flexeril cyclobenzaprine vs cialis
Pingback: online order dutasteride cheap united states
Pingback: androxal walmart price
Pingback: enclomiphene online in australia
Pingback: canada pas cher kamagra